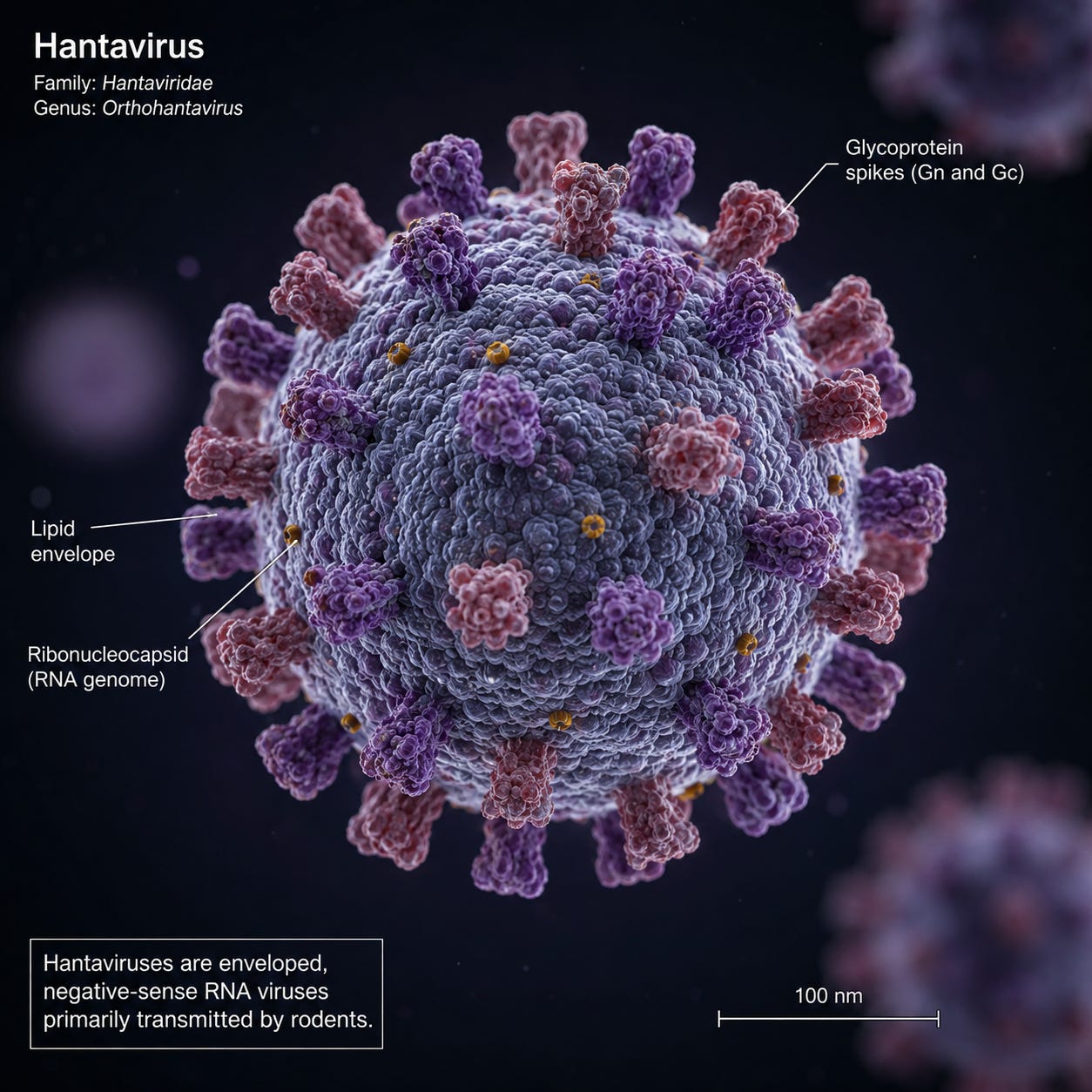
Hantavirus and the cruise ship outbreak: What it really means for you
Don't worry too much about the ship, but watch out for mice and rats
When headlines talk about a “deadly hantavirus” on a cruise ship, it’s easy to feel a familiar jolt of dread. Another pandemic? Another virus spreading silently through airports and grocery stores?
Health officials say no.
A rare outbreak of hantavirus tied to a cruise ship in the Atlantic has killed several passengers and sent others to hospitals around the world, including the United States, but experts stress that the risk to people who were not on that ship is extremely low.
For most Americans, the more realistic hantavirus risk has nothing to do with cruise lines or foreign ports. It’s much closer to home—living in garages, sheds, and cabins, wherever mice and other rodents have settled in.
So what should you actually do?
How to protect yourself
1. You do not need to overhaul your life because of this outbreak
There is no recommendation for Americans to change everyday routines—school, work, shopping, social events—because of this cruise‑ship cluster. Health agencies describe the risk to the general public as “very low” or “extremely low,” because the known cases all trace back to one ship and a limited group of passengers and crew, according to the Centers for Disease Control and Prevention (CDC).
If you were not on that vessel and haven’t had close, prolonged contact with someone who was, you do not need special testing, monitoring, or quarantine. Normal good‑sense health habits — staying home when you’re sick, washing your hands, getting care if you have serious symptoms—still apply, but there are no hantavirus‑specific restrictions for the general public.
If you are planning a cruise or international trip, the most practical step is simple: check official travel‑health information before you go and again shortly before you return, the way you might check the weather. If guidance changes, that’s where it will show up first, the World Health Organization advises.
2. Make your home less friendly to mice and rats
Where hantavirus is concerned, rodents — not crowds — are the main problem.
In the U.S., officials have traced most past hantavirus infections to encounters with wild rodents, especially deer mice and related species, in and around homes, cabins, sheds, and workplaces. The virus lives in rodent urine, droppings, and saliva, and people usually get infected by breathing in tiny particles from those materials after they dry and get stirred into the air.
Public‑health guidance boils down to a few simple steps:
Seal entries. Close gaps and holes in foundations, walls, roofs, and around pipes or vents where rodents can squeeze in. Remember that mice can slip through openings much smaller than you might expect.
Store food smartly. Keep human and pet food in sturdy containers with tight‑fitting lids. Clean up crumbs and spills quickly, and don’t leave pet food out all night.
Manage trash. Use trash cans with tight lids, and if possible, store them away from doors and windows. Don’t let garbage or recycling pile up in corners where rodents can hide.
Cut clutter. Piles of cardboard, firewood, and junk near the house make great nesting spots. Moving them away from the home and off the ground makes life harder for rodents.
Use traps when needed. Snap traps — used carefully and kept away from kids and pets — are a recommended method for indoor rodent control. For bigger infestations, it may be safer and more effective to hire a pest‑control professional.
These aren’t just hantavirus measures; they’re general home‑health measures that also reduce the risk of other rodent‑borne problems.
3. Clean droppings and nests the right way
The single most important “how‑to” for hantavirus is how not to clean.
The instinctive reaction when you see mouse droppings on a garage floor is to grab a broom or a shop‑vac. That’s exactly what experts say not to do. Dry sweeping and vacuuming can launch tiny contaminated particles into the air, which you can then breathe deep into your lungs.
Here’s the method recommended by public‑health agencies:
Ventilate first. If you can, open doors and windows for about 30 minutes before cleaning, and step out during that time so fresh air can circulate.
Protect yourself. Put on rubber or plastic gloves. For heavy infestations or very dusty spaces, a well‑fitting mask or respirator can provide added protection.
Wet, don’t sweep. Thoroughly soak droppings, urine, and nests with a household disinfectant or a bleach solution (for example, 1 part household bleach to 10 parts water). Let it sit for at least 5 minutes.
Wipe up. Use paper towels or disposable rags to pick up the soaked material. Place everything into a plastic bag.
Disinfect surfaces. Mop or wipe the area again with disinfectant or bleach solution.
Dispose and wash. Seal the trash bag and throw it away. Remove your gloves and wash your hands thoroughly with soap and water.
If you walk into a space that’s clearly heavily infested — lots of droppings, strong odors, visible nests—it may be safer to call in professionals who have protective equipment and experience with this kind of cleanup, especially if you have underlying lung problems.
4. Take extra care with cabins, sheds, and campers
Many documented hantavirus cases in the U.S. have been associated with rustic cabins, vacation homes, sheds, barns, and similar structures that sit unused for long periods. These spaces are irresistible to rodents: quiet, sheltered, and full of nesting material.
Before spending a night in a cabin or camper that’s been closed up for months, it’s wise to:
Open the doors and windows, and air it out.
Look for droppings, nests, or gnaw marks along baseboards, cupboards, and bedding.
Clean using the “wet, don’t sweep” method if there are signs of rodents.
Wash any bedding or soft furnishings that might be contaminated.
Campers and hikers should keep food tightly sealed, avoid sleeping directly on bare ground where droppings are visible, and avoid disturbing obvious rodent nests.
5. Know when to call a doctor—and what to say
Hantavirus often starts like a garden‑variety flu: fever, fatigue, and muscle aches, sometimes headache or stomach upset. What makes it different — and dangerous — is that for some patients, it can quickly progress to breathing problems and low blood pressure as the lungs begin to fill with fluid.
Public‑health officials advise you to seek medical care promptly if both of these are true:
In the past one to five weeks, you had significant rodent exposure—cleaning heavy droppings in a closed space, working in a rodent‑infested building, or staying in a cabin with obvious signs of mice or rats; and
You’ve developed fever, fatigue, body aches, and especially new or worsening shortness of breath or a feeling that you can’t catch your breath.
If you do see a doctor or visit an emergency room, it helps to say the quiet part out loud: “I’m worried about hantavirus because I was cleaning up a lot of mouse droppings.” That clue can prompt the right tests and infection‑control measures. Early supportive care in a hospital—oxygen, close monitoring, and intensive care for severe cases—can improve outcomes.
What’s actually happening on that cruise ship?
With the practical advice in hand, it’s worth stepping back to look at the outbreak that put hantavirus into the headlines.
A rare cluster at sea
In early May, international health officials were alerted to a cluster of passengers with severe, unexplained respiratory illness aboard the MV Hondius, a small expedition cruise ship operating in the Atlantic Ocean. At that point there were 147 passengers and crew from 23 countries on board; 34 others had already left the ship earlier in the voyage.
Several passengers rapidly became critically ill, and at least two died before the ship reached port. Testing confirmed that the cause was a hantavirus. A few days later, the specific culprit was identified: Andes virus, a type of hantavirus previously known from South America.who+5
By the time the World Health Organization issued its first detailed update, eight cases linked to the ship had been reported—six confirmed and two suspected—including three deaths. As more passengers were evacuated and tested in hospitals around the world, that number grew; subsequent tallies described 11 confirmed cases tied to the voyage, still with three fatalities.khou+2
Americans under observation
The story became a domestic concern when it emerged that Americans were among those on board and had been exposed.
News outlets reported that 18 American passengers were flown back to the United States after the ship docked near Spain’s Canary Islands. Sixteen went to a biocontainment and monitoring facility in Nebraska, and two were sent to Atlanta. At least one of those travelers tested positive for Andes virus; another had mild symptoms but was under observation.
At the same time, health officials discovered that several Americans had already disembarked earlier in the trip and returned home before anyone realized a serious outbreak was underway. The Centers for Disease Control and Prevention alerted state health departments in the relevant states, who then contacted those travelers to advise them on symptom monitoring and to arrange testing if needed.
No sign of wider spread
Despite the dramatic images of a “virus‑stricken cruise ship,” multiple health agencies have delivered a consistent message: this is a contained, unusual event, not the beginning of a broad wave of infections.
CDC’s official situation summary states that there is no evidence of ongoing person‑to‑person transmission in U.S. communities linked to the cruise, and that the risk to the general public remains extremely low. The World Health Organization and the European Centre for Disease Prevention and Control have reached similar conclusions for their regions, calling the risk to the general public “very low.”
In plainer language: unless you were on that ship—or living in close quarters with someone who was and is now sick—this outbreak does not change your personal risk in any meaningful way.
So what is hantavirus, really?
Hantaviruses are not newcomers. They’ve been on scientists’ radar for decades.
A brief history
The first recognized human disease caused by a hantavirus was documented among soldiers during the Korean War in the early 1950s, when thousands developed a severe illness known as Korean hemorrhagic fever. It took years for researchers to identify the responsible virus and connect it to its rodent hosts.
In the Americas, hantavirus burst into public awareness in 1993, when an outbreak of unexplained acute respiratory failure among young, otherwise healthy adults hit the Four Corners region where Arizona, New Mexico, Colorado, and Utah meet. Investigations eventually traced those cases to a previously unknown hantavirus carried by deer mice, leading to the description of hantavirus pulmonary syndrome as a distinct disease.news.
Since then, sporadic cases and occasional small clusters have been reported each year in North and South America, Europe, and Asia—usually in rural areas where people live or work in close proximity to rodent reservoirs. It almost never looks like a flu or COVID‑style wave; instead, it appears as individual tragedies and small outbreaks.
Two main disease patterns
Globally, hantaviruses cause two primary clinical pictures:cdc+2
Hantavirus pulmonary syndrome (HPS/HCPS) – Seen mainly in the Americas, this form starts with fever and fatigue and can progress to severe lung involvement and shock. Case‑fatality rates in some series have reached around 30–50 percent.news.
Hemorrhagic fever with renal syndrome (HFRS) – More common in parts of Europe and Asia, this form affects blood vessels and kidneys, ranging from mild illness to severe disease with kidney failure and bleeding.
The specific outcome depends in part on which hantavirus species is involved and which rodent carried it. Different regions have different rodent reservoirs, and different reservoirs carry different virus types.
Why Andes virus is a special case
Most hantaviruses do not spread meaningfully from one person to another, experts say. When someone becomes sick, the usual source is a rodent, not another human.
Andes virus, the type behind the cruise‑ship outbreak, is one of the few known exceptions. Studies from South America have documented limited human‑to‑human transmission in close‑contact settings, such as among household members or healthcare workers caring for very sick patients.
Even then, the virus does not spread easily the way airborne viruses like measles or highly contagious respiratory viruses like SARS‑CoV‑2 do. But it does require an extra layer of caution, especially in confined environments and hospitals.
That is why, once Andes virus was identified on the ship, health authorities moved quickly: evacuating passengers, isolating patients, tracing contacts, and issuing guidance for hospitals on using airborne precautions like N95 respirators and special ventilation rooms when caring for suspected cases.
Who’s in charge of keeping it that way?
For an American audience, it helps to know there’s a system behind the scenes.
The Centers for Disease Control and Prevention (CDC) leads the U.S. response, from investigating cases and coordinating with state health departments to issuing alerts to doctors and hospitals.
State and local health departments handle the on‑the‑ground work: contacting travelers, arranging testing, and providing information to communities.
The World Health Organization (WHO) coordinates between countries, sharing data and advice, and helps make sure that the response in one place doesn’t leave gaps elsewhere.
European and other national agencies oversee evacuees and cases in their regions, with assessments so far mirroring the U.S. message that risk to the general public is very low.
The system isn’t perfect, but it is there—and for a virus like hantavirus, which moves slowly and rarely in human populations, that’s usually enough to prevent isolated outbreaks from becoming something larger.
The bottom line
The words “deadly virus” and “cruise ship” in the same sentence will always grab attention. In this case, the danger is very real for the small number of people who’ve become sick—and for their loved ones. But for most Americans, the immediate takeaway is surprisingly practical and unglamorous:
You don’t need to panic about cruise ships or airports because of hantavirus.
You do need to pay attention to mice and rats in the places you live, work, and vacation.
A few simple steps—rodent‑proofing your home, cleaning droppings safely, and getting prompt care if you get sick after heavy rodent exposure—go a long way toward keeping this rare, serious illness exactly that: rare.cdc+3